Breath analysis can detect distinctive metabolic changes that are among the earliest signs of disease. But could it one day replace blood tests for certain conditions? Katrina Megget reports
‘Would you rather go to hospital for an invasive, embarrassing or painful procedure, like a colonoscopy, or stay at home and send some of your breath away in a tube to be analysed?’ Billy Boyle, co-founder of Owlstone Medical, a Cambridge, UK-based biotech, believes breath analysis is the non-invasive and cost-efficient answer to improve early disease detection and prevent untimely deaths. The company is one of a growing number of firms and research labs exploring the chemistry of exhaled breath and developing sensors and devices to capture and analyse it to help diagnose disease.
The interest is based on the fact human breath contains more than 1000 volatile organic compounds (VOCs), originating either from diet, drugs and environmental exposure to pollutants, or in the body via cellular metabolism. Research suggests diseased cells have an altered metabolism compared with healthy cells, and recent discoveries have shown correlations between concentrations of VOCs and different diseases. For instance, elevated acetone is a strong indicator of diabetes, while several aldehydes may indicate lung cancer, and undecane, 3-methylhexane and 1-pentadecene could reflect airway inflammation in respiratory diseases.
The thinking goes these VOC differences could be diagnostic breath biomarkers for a range of diseases. Given that metabolic changes can be some of the earliest signs of disease, there is potential for breath analysis to detect illnesses without any prior knowledge of what diseases are present or where in the body they are active.
Since 2000, the concept of breath analysis has gained traction thanks to progress in spectrometry and sensor technology. Now the field is entering a new phase of maturation with the promise of simple non-invasive breath tests, possibly performed and analysed at home, with results delivered faster than a blood test. In November 2021, The World Economic Forum listed breath analysis as one of the top ten breakthrough technologies with the potential to significantly impact the world.
Boyle agrees, saying Owlstone’s mission is to save 100,000 lives and $1.5bn in healthcare costs. ‘The difference that breath analysis could make is in lowering the barrier to healthcare, helping more people to get help when it can make a real difference to their future.’
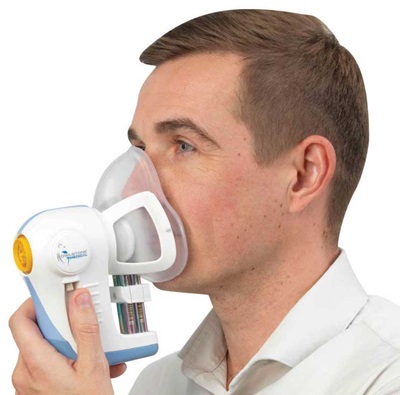
Owlstone looks to achieve this by discovering specific breath biomarkers through its ReCIVA Breath Sampler collection device and GCMS. A person breathes into the handheld device through a snorkel-like mouthpiece, with the breath collected in a cartridge. The ambient VOCs from inhaled air are removed to reduce background signals and improve sensitivity, while VOC analysis occurs in the lab, separating and identifying VOCs in the parts per trillion range. ‘We strongly believe that detecting specific VOCs is essential to developing tests that can be successfully developed for clinical use,’ says Boyle, who hopes to establish a database or breath biobank of VOCs correlated with disease.
Uncovering cancer
In an upcoming study of 88 people, Owlstone improved the ability to detect limonene and identified other compounds. The study also showed the most notable compounds change in relation to disease severity and other markers of reduced liver function, which could make them effective for detecting earlier stages of liver disease, Boyle says. These findings have led the company to develop exogenous VOC probes whereby, for example, limonene, found in citrus, can be administered to a patient and its metabolism measured in the breath to detect liver disease.
Meanwhile, in another project looking at lung cancer in former smokers, Owlstone detected several promising aldehyde and alkane compounds that may be related to a process called lipid peroxidation, associated with cellular stress.
We strongly believe that detecting specific VOCs is essential to developing tests that can be successfully developed for clinical use.
Billy Boyle co-founder, Owlstone Medical, Cambridge, UK
Sensor development
For Boyle, breath biomarkers are the key for next generation breath analysis. GCMS is considered the gold standard in analysis, but it is lab-based and expensive. For this reason, many see the development and use of small, portable sensors as the future. ‘Sensors offer many benefits for clinical use and they are likely to feature in the future of breath tests in the clinic,’ Boyle says, but he believes that knowing the identity of biomarkers is needed to construct optimised sensors to diagnose disease.
However, a lack of validated biomarkers hasn’t stopped development in the sensor space. Essentially, the sensor is a chemically active surface tuned to specific compounds and connected to an electrical system. When the compound interacts with the surface, it produces a signal, explains Paul Thomas, Professor Emeritus of analytical science at Loughborough University, UK, and board member of the International Association of Breath Research. The advantage of sensors is they are small, fast, and easy to use, with analysis made at point-of-care.
Sensor devices – often called electronic noses or e-noses – can contain many different sensor arrays. This allows the sensor to pick up a pattern of different VOCs as a ‘fingerprint’ of a disease, similar to how the mammalian olfactory system works. Artificial intelligence is often used for real-time pattern recognition to match measured patterns to previously seen ones.
Metal-oxide semiconductor-based sensors are particularly popular. These sensors are based on a temperature-dependent redox reaction in response to VOCs, which creates a change in electrical conductivity of the oxide material that can be measured. Examples of metal oxides include tungsten oxide and molybdenum oxide. Other possible breath sensors have included metal-oxide composites with carbon nanotubes, graphene and noble metal nanoparticles.
Electrochemical sensors are also gaining interest in breath analysis. Here the VOCs are oxidised or reduced on an electrode surface, such as gold, graphene or platinum black-coated Teflon. The transfer of electrons that takes place as a result of the redox reaction flows through an external circuit and generates a signal. The electron flow creates an electric current proportional to the concentration of the VOCs.
There are also various other types of sensors being considered, such as colorimetric sensors that change colour in the presence of target VOCs, piezoelectric sensors that measure the change in oscillation frequency of a quartz crystal microbalance when it absorbs VOCs, and lasers, among others.
Solving challenges
However, wide scale adoption of breath analysis still presents several challenges. One is improving the detection accuracy, especially the algorithms that analyse the sensor data. ‘One of the challenges of breath analysis is we don’t have enough data yet for AI to help us,’ says Thomas, adding that around 25,000 samples are needed to boost AI’s capabilities.
In addition, standardised breathing protocols and guidelines are needed. Boyle notes there are many ways to study breath, but these can produce differing results, making comparison across studies difficult. Better comparison is needed to spot patterns and identify biomarkers, he says.
Perhaps one of the biggest challenges is factoring in the confounding effect of co-morbidities, diseases with similar symptoms or even nuanced differences between people, says Thomas. ‘It’s a bit like looking at the sun and looking for a flashing light. There’s a lot of background noise.’ Owlstone’s breath biobank is one way to fine-tune this with specific breath biomarkers.

Similarly, a team at Radboud University in The Netherlands used breath analysis in a study of 400 adults scheduled for an endoscopy. Of those adults, 129 had Barrett’s oesophagus, a precursor to oesophageal cancer, 141 had acid reflux disease and 132 had a normal oesophagus or hiatus hernia. ‘The belief is Barrett’s oesophagus and reflux are closely associated [with similar symptoms],’ says Peter Siersema, Professor of endoscopic gastrointestinal oncology, who led the study. ‘I was at first sceptical that an e-nose would pick them up, but the results are fantastic – it distinguished between the two as two distinct and very different disorders.’
The study used a commercial sensor by The eNose Company, which contains three metal-oxide sensors. It showed the VOC profiles differed significantly between the three groups of participants, while the sensitivity of picking up Barrett’s oesophagus was 91% and the ability to detect those without the condition was 74%. In addition, the taking of proton pump inhibitor drugs to curb stomach acid production, which can suppress symptoms, made no difference in terms of accuracy.
While further research is required to validate the findings, Siersema says the results point to a new way to diagnose the precursor to oesophageal cancer. ‘This has the potential to reduce the number of patients being referred to hospital and provides the ability to detect more patients at early stages. That will lead to reduced numbers of patients with advanced disease, which will lead to reduced healthcare costs.’
Other avenues
Beyond diagnosis, breath analysis also holds promise in other applications. This includes monitoring disease and progression, infectious disease control, highlighting elevated markers of an unhealthy lifestyle, and measuring exposure to hazardous substances and pollutants, says Thomas. There is scope that breath analysis might even replace blood tests in some cases and it may also play a role in countries with limited diagnostic resources.
Another potential application concerns personalised medicine. Here, breath biomarkers could predict therapy response, treatment efficacy and even the potential for side effects. Owlstone is already investigating metabolic rates for the CYP450 liver enzymes, which influence the efficacy of many common drugs. Meanwhile, another team at Radboud University used an e-nose developed by Breathomix to identify, with 85% accuracy, lung cancer patients who will and will not respond to immunotherapy. The results are now being clinically validated.
Siersema envisages a future where one device will detect different diseases in the space of 10 minutes - and hopes it could be available in GP surgeries in as little as three to five years. Meanwhile, Boyle foresees a networked device that people blow into everyday to generate health data. ‘What excites me the most is that I don’t see limits to how breath could be used in healthcare.’
Breath sensor for Covid
In Israel, Hossam Haick, Head of the Laboratory for Nanomaterial-Based Devices at Technion – Israel Institute of Technology, is exploring portable molecularly modified chemical sensors, which received an EU Innovation Award in 2018. These comprise a flexible, thin film of gold nanoparticles linked to electron withdrawing and donating organic ligands. The film is placed onto a flexible polyimide substrate, which sits between two electrodes. ‘The sensors create a diverse sensing layer that can swell or shrink upon exposure to volatile organic compounds, causing changes in electrical resistance,’ he says. ‘Different sensors can be used, depending on the functional groups, to create an array of cross-reactive, semi-selective sensory units that mimic mammalian olfactory systems that pick up a disease VOC pattern rather than a specific VOC.’
Haick’s team has studied the sensor in a variety of cancers, as well as liver and kidney disease and tuberculosis. In ovarian cancer, it correctly diagnosed the disease in 82% of patients. Now Haick has turned his sensor’s attention to Covid-19. His team trained the sensor to detect the viral infection by using machine learning to compare the pattern of electrical resistance signals obtained from the breath of confirmed Covid patients in Wuhan, China, with those from healthy controls and those with non-Covid lung infections.
Once machine learning identified a potential Covid-19 signature, the team tested the accuracy of the device on a subset of participants. It achieved 76% accuracy in distinguishing Covid-19 cases from controls and 95% accuracy in differentiating between patients with Covid-19 and those with other lung infections. The sensor could also distinguish with 88% accuracy between sick and recovered Covid-19 patients.
‘One advantage is the potential for a fast point-of-care test, needed in the era of global pandemics,’ Haick says. Such a device could be rolled out at airports, shopping centres, and hospitals for rapid large population screening and to detect asymptomatic contagious individuals, he says.





